This story was written by Subhashree in her own words. Names have been changed to protect privacy. Published with the couple’s consent.
A note from Fertilia: What follows is Part 1 of Subhashree’s journey: from trying to conceive, through a miscarriage, a low AMH diagnosis, and a failed IUI, to natural conception with Fertilia. Part 2 continues the story through her pregnancy, normal delivery and postpartum. We have kept her words as she wrote them. Dr. Suganya has added clinical observations at the points where they mattered most. We are deeply grateful that Subhashree and Kathir chose to share every part of this story, including the parts that were hardest.
Finding Our Way Back to Hope
I’m Subhashree, 32, a teacher currently on a break and doing online tutoring. My husband Kathir, also 32, is a fashion designer. We’ve been married for four years, and like many couples, we always believed starting a family would happen naturally, in its own time.
After settling into married life, we reached a phase where starting a family felt natural and exciting. We began trying to conceive from the third year of our marriage, holding on to the simple belief that it would happen in its own time.
In 2022, I was diagnosed with an ovarian cyst, which was the first time we felt a small pause in what we had always imagined would be a simple and natural journey.
The Miscarriage We Never Expected
As we slowly moved forward from that phase, holding on to hope, in early 2023 I conceived naturally. For a brief moment, everything felt right and we experienced a quiet sense of happiness.
But that phase did not last long. We went through a miscarriage, followed by an MTP. It wasn’t just the loss that hurt, but the feeling of having something so real, so close to us, and then suddenly losing it. In many ways, it felt even more painful than not conceiving at all, because for a moment we had felt that life within us, and then it was gone. It’s a kind of pain that quietly stays within, something we found very difficult to put into words.
That experience left us emotionally drained. While we tried to stay strong and move forward, it was not easy to come out of that phase and start again with the same confidence.
Low AMH, Follicular Study, and an IUI That Could Not Happen
As time went on, we continued exploring medical options, hoping to understand what was causing the delay. My AMH levels were low, which made us more conscious about time and possibilities. We went through a follicular study in November 2024, followed by an IUI in December 2024.
The IUI did not go the way it was supposed to. During the procedure, the doctor told us that my cervical opening was very small and the IUI catheter could not go inside the uterus. That moment shook both of us. We had walked in hoping for an answer. We walked out with a new question, and a very frightening one: if a thin catheter could not pass through, how would a baby ever come out?
With every step, we held on to hope, telling ourselves that maybe this time it would work. But when it didn’t, the disappointment was not just about the result. It was about the emotional effort that came with each attempt.
Slowly, stress and anxiety started becoming a part of our everyday life. There were so many questions, but very few clear answers. The waiting, the uncertainty, and the repeated cycles of hope and disappointment began to take a toll on us.
During this phase, I also began to realise that while I was going through everything physically, Kathir was carrying his own share of this journey in a much quieter way. He stood by me through every step, staying strong and supportive, even when things were not easy.
We were told that if IUI had not worked, IVF would be the next step. And as human nature does in a moment like that, part of us wanted to rush toward it, just to put a full stop to the uncertainty. But another part of us was not ready. Not physically, not mentally, not emotionally.
Choosing to Pause Instead of Rush
That’s when we felt the need to pause. Not because we were giving up, but because we wanted to understand if we were truly approaching this in the right way.
We decided to step back and reflect on what our bodies truly needed. Instead of continuing with repeated attempts, we wanted to focus on building a stronger and healthier foundation, physically, mentally, and emotionally. With that clarity, we chose to approach Fertilia, looking for a more balanced and supportive way to move forward.
What the Reports Showed
During the initial consultation, both of us were equally acknowledged, and our complete history was understood in detail. We were then guided to undergo a few basic investigations to gain clarity on what was happening internally.
The reports gave us a much clearer picture of what our bodies were lacking and where the gaps were.
In my case:
- My AMH was 1.63 ng/mL, indicating a lower ovarian reserve for my age
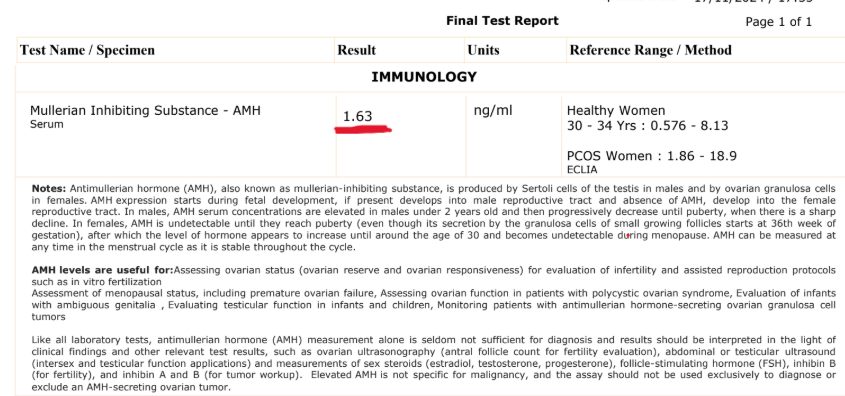
- Prolactin was elevated at 31.61 ng/mL (normal range: 4.60 – 25.07 ng/mL), which could interfere with normal hormonal balance and ovulation

- Vitamin D3 was significantly low at 19.15 ng/mL, in the deficiency range, pointing to an overall deficiency that needed correction

At the same time, Kathir’s reports also highlighted important aspects. His sperm morphology was significantly affected, with only a very small percentage of normal forms. Motility was also not at an optimal level. It wasn’t something he had expected, nor something he had ever physically felt, but suddenly it mattered.
When we looked deeper into his IUI semen analysis report, the picture became clearer:
- The sperm count was adequate
- Only about 1% of the sperm were structurally normal, meaning most were not capable of effective fertilisation (a diagnosis of teratozoospermia, with elongated and amorphous head defects)
- There was increased viscosity, making movement more difficult
- Motility improved after processing, but it could not compensate for poor morphology
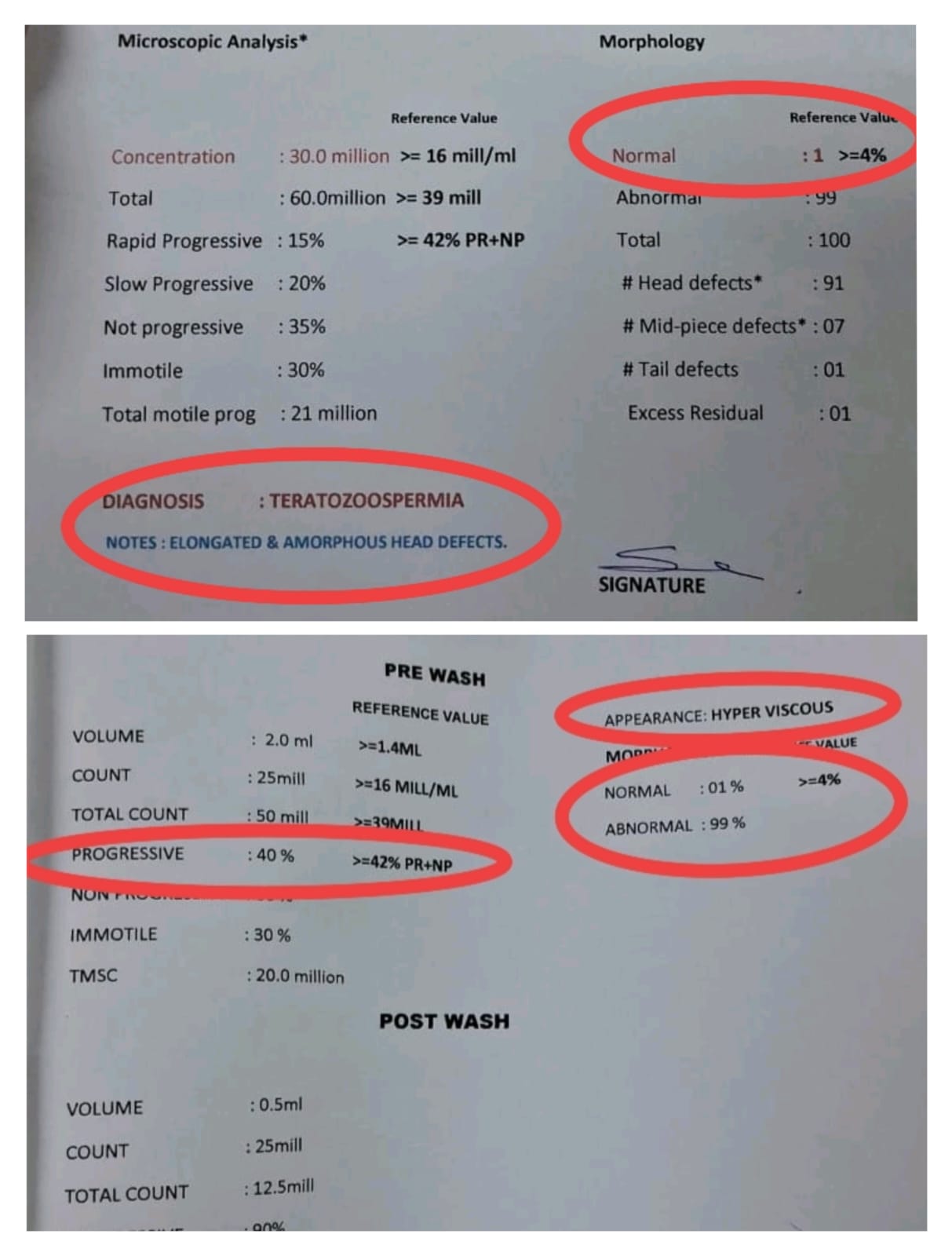
These findings made us realise that fertility was not just about numbers. It was about how well the body was functioning overall. The delays were not without reason. Both of us needed the right kind of support and correction.
The direction we chose at that point felt different. It was not about rushing into treatments. It was about slowly rebuilding balance in our lifestyle.
Dr. Suganya’s note
This couple came to us after four years of marriage. The main issue was that IUI had been recommended because of borderline sperm parameters. The IUI was not successful, and on top of that, the doctor told them the cervical opening was very small and the IUI catheter could not go inside the uterus at all. They were dejected, thinking that if IUI had not worked, then IVF was the only path.
But before proceeding with any invasive fertility treatment, they wanted to try Fertilia’s holistic fertility optimising program first. During the program we supported her clinically and nutritionally, but just as importantly, we helped reduce the stress both of them were carrying. And to everyone’s surprise and happiness, she conceived naturally one and a half months into the program.
The Program: Small, Sustainable Steps
We realised that what we needed was the right nutritional support, and that’s when we were guided through a nutrition consultation followed by a personalised meal plan that felt practical and suitable for our routine.
We began focusing on a fertility-friendly way of eating that suited our routine and preferences. Simple changes, like consciously including millets at least three times a week, having one fruit a day, and making small, consistent adjustments that felt manageable and sustainable rather than overwhelming.
Alongside this, simple physical activity became part of our routine. Even though I was at a normal and ideal weight for my height, the focus was on what my body specifically needed at that time: improving flexibility, strength, and overall balance, rather than doing intense workouts.
Equal importance was also given to emotional well-being. Through small mindful practices, we slowly started feeling more calm, grounded, and connected to the process, rather than constantly feeling anxious about the outcome.
The Changes Came Quietly
Within the first month itself, I got my periods, which felt like a reassuring start. Gradually, small changes became noticeable: my energy levels improved, and even concerns like dandruff started reducing.
By the second month, the changes felt more visible, not just physically, but mentally as well. I felt calmer, less anxious, and more at ease with the process. For the first time in a long while, the journey didn’t feel rushed or pressured.

We continued this way, focusing on small, consistent efforts rather than constantly thinking about the outcome. And then, in a way that felt natural and unforced, something we had been hoping for happened.
I conceived.
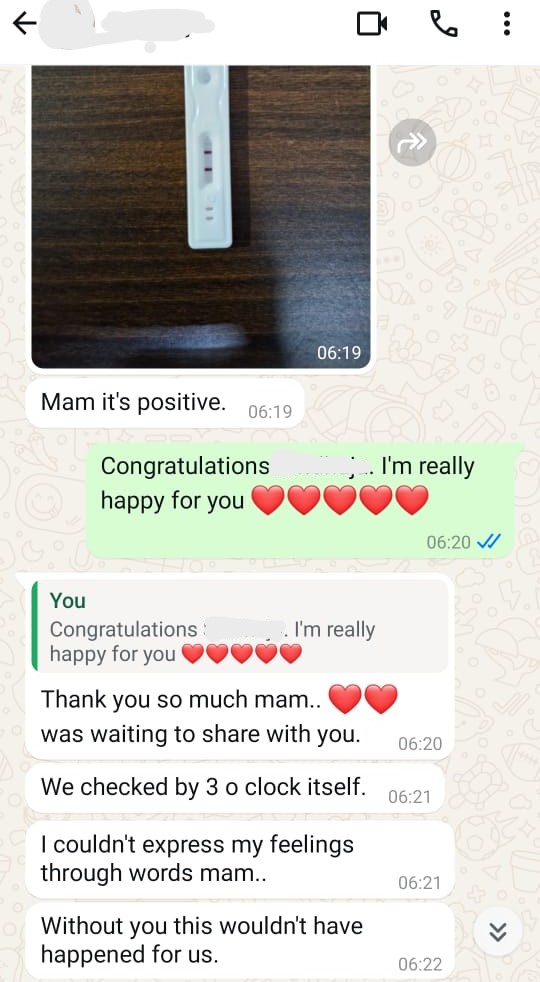
From a phase that began with an ovarian cyst, continued into natural conception followed by a miscarriage, then a low AMH diagnosis, a follicular study, and an IUI that could not even be completed because of my cervix, this journey had many ups and downs. But what truly made a difference was the clarity in how we chose to approach it. Instead of constantly looking outside for answers, we began understanding what our bodies truly needed, and started taking care of ourselves in a more mindful and consistent way.
With the right kind of support, we were able to focus on what was actually required for our bodies, rather than doing everything at once. That approach helped us feel more aligned, balanced, and confident as we moved forward.
And somewhere along the way, things gently began to fall into place, step by step, bringing us closer to the moment we had been hoping for.
The story continues
Subhashree’s pregnancy, normal delivery, and postpartum story is told in Part 2, including how she prepared for labour, the night her labour started, and the “show” that told her it was time.
Are You in a Similar Situation?
If you’ve been told that IUI or IVF is your only option, or if a previous treatment has not worked, Dr. Suganya and her team can help you understand whether a structured lifestyle window is worth trying first, or whether assisted reproduction is genuinely the right next step.
Frequently Asked Questions
Is a failed IUI an indication that I should move straight to IVF?
Not always. An IUI may fail for several reasons: a poorly timed cycle, a mismatch between the husband’s morphology and what IUI is designed to overcome, or a technical issue on the day of the procedure (such as a cervix that was difficult to access). IVF may eventually be the right step, but for a couple whose semen parameters sit in the borderline range, and where lifestyle, hormones, and ovulation have not been optimised yet, a structured lifestyle window of 2 to 3 months is often worth trying first. It can also prepare the body better if IVF is eventually needed.
Can a woman with low AMH conceive naturally?
Yes. AMH tells you how many eggs are left, not the quality of any particular one. A woman with low AMH has a smaller runway and less time to work with, which is why waiting passively is not a good strategy. But a low AMH does not mean conception is impossible. Subhashree’s AMH was 1.63 ng/mL when she reached us, which is below the healthy range for her age, and she conceived naturally within six weeks of starting the program. For a deeper look at the numbers and what they actually mean, see our guide on how to increase AMH levels naturally.
Does sperm morphology really matter if the count is normal?
Yes. Morphology (the shape of the sperm) is a measure of how many sperm are structurally capable of fertilising an egg. Kathir’s semen analysis showed a normal total count but only 1% normal forms, with elongated and amorphous head defects. This pattern is called teratozoospermia. Sperm with head defects often cannot bind to the egg or penetrate it properly, which is why even a “high count” can still result in failed IUIs or unexplained infertility. Morphology responds to lifestyle. Improvements in nutrition, sleep, hydration, heat exposure, and antioxidant status can all shift morphology over 2 to 3 months (the time it takes for new sperm to form). This was a big part of the focus for Kathir.
How soon after a miscarriage is it safe to try again?
There is no single answer, and it is as much emotional as it is physical. Physically, most women can try again after one or two regular periods, provided there are no retained products and no complications from the miscarriage (or the MTP procedure, if one was done). Emotionally, some couples are ready quickly, others need months. Subhashree and Kathir took time to rebuild, physically and emotionally, before starting again, and that turned out to matter. Our full guide on miscarriage causes, signs, and recovery goes into this in more detail.
What does the Fertilia program actually include for a couple like this?
A typical couple’s program includes: a detailed initial consultation with Dr. Suganya to understand history and goals, a set of relevant investigations for both partners (not a generic panel), a personalised nutrition plan built around your routine and food culture, a trimester-aware activity plan, emotional and mental wellness support with affirmations and reflection practices, regular check-ins, and a clear threshold for when assisted reproduction is the right next step. If pregnancy happens, the same team continues with trimester-wise care, antenatal yoga, labour preparation, and postpartum plus lactation support. This is what Subhashree and Kathir went through. Part 2 of her story walks through the pregnancy side.
Every Journey Starts with a Conversation
Whether you’re trying to conceive, recovering from a miscarriage, preparing for IUI or IVF, or navigating pregnancy, Dr. Suganya and her team are here to understand your unique situation and walk with you through every phase.
This story is part of Fertilia’s “My Journey” series, where past patients share their experiences in their own words. Every story is real, verified, and published with the patient’s explicit consent. Names have been changed to protect privacy.
Continue reading: Part 2 · From Conception to Normal Delivery: Subhashree’s Pregnancy Journey




