Names have been changed to protect patient privacy. Clinical details and images are shared with the patient’s consent.
Fertility journeys are rarely equal in how they are seen. The woman’s pain is visible: the injections, the reports, the hormones, the tears. But a man’s experience often stays within. Vikram’s journey was one of those quiet stories.
The Weight He Carried Silently
Vikram, a 32-year-old fashion designer, spent most of his days sitting. Creating, meeting deadlines, constantly switched on mentally. It was a routine that looked productive on the outside, but over time, his body adapted to a pattern of low movement, irregular meals, and underlying stress. Nothing felt wrong. No symptoms, no clear signs. Not until life began to ask more from his body.
When Swathi and Vikram began trying, the focus shifted to her, as it usually does. And her journey was not easy. An ovarian cyst in 2022, followed by a pregnancy in 2023 that ended in a miscarriage and then an MTP. Each experience took an emotional and physical toll. Vikram stood by her through all of it, watching her go through pain, loss, and recovery.
Then came the reports. Low AMH, high prolactin, severely low Vitamin D. Each number added more weight to their journey. They continued trying through treatments, follicular studies, and repeated cycles of hope. Through all of this, Vikram watched her go through more, physically and emotionally. He didn’t express much, but he felt everything.
By the time they reached IUI, exhaustion had already settled in.
When His Report Came Into Focus
IUI brought a shift. For the first time, it wasn’t just about her body anymore. That’s when Vikram’s reports came into focus.
His semen analysis did not show a problem with count. The numbers were within range. The concern was in quality.
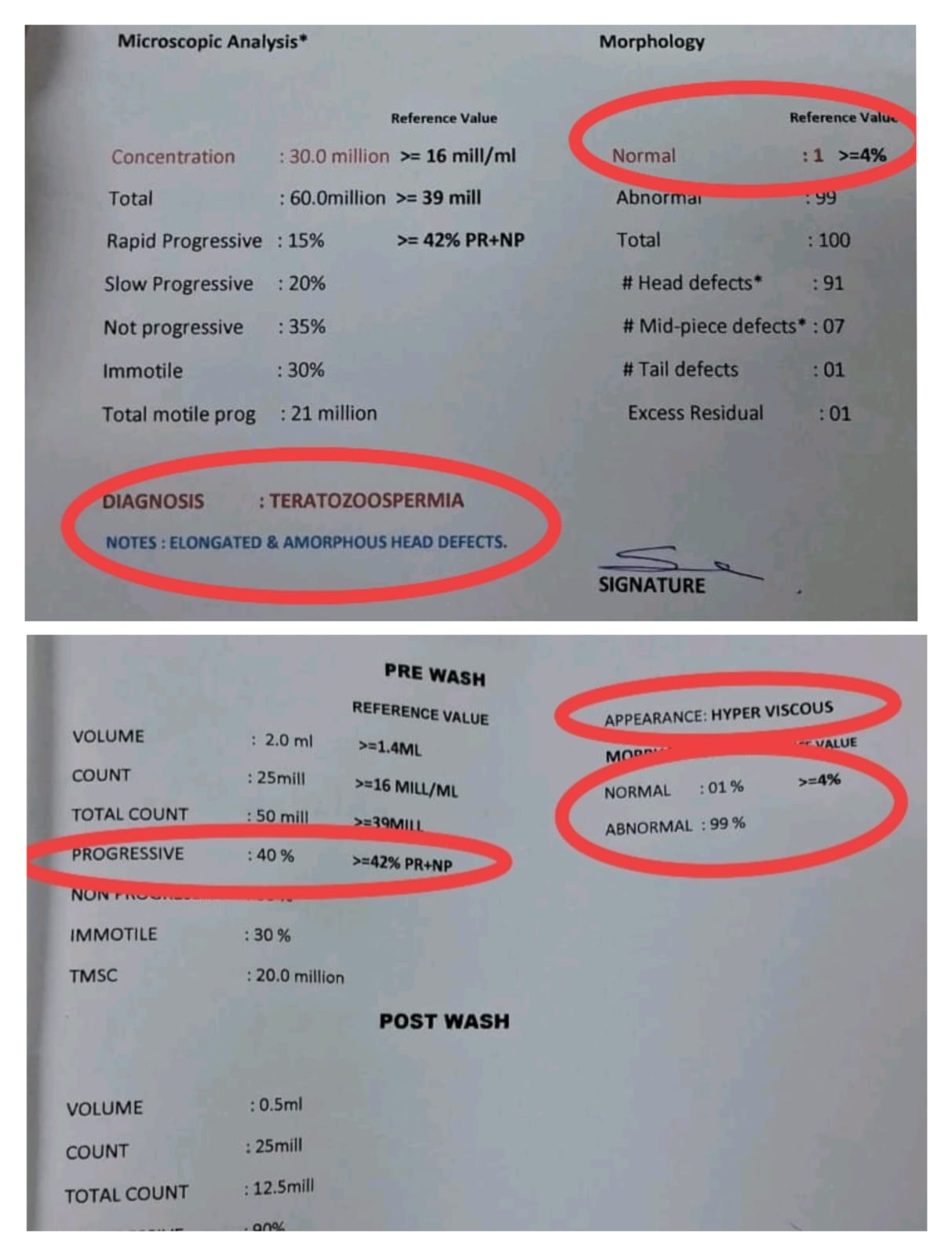
Here’s what the report showed:
Microscopic analysis:
- Concentration: 30.0 million/mL (reference: 16 million or more)
- Total count: 60.0 million (reference: 39 million or more)
- Progressive motility: 35% (reference: 42% or more for total progressive)
- Immotile: 30%
Morphology (the critical finding):
- Normal forms: 1% (reference: 4% or more)
- Head defects: 91 out of 100
- Diagnosis: Teratozoospermia
IUI pre-wash sample:
- Appearance: Hyper viscous (making movement more difficult)
- Normal morphology: 1% (unchanged)
- Progressive motility: 40% (slightly below the 42% reference)
It wasn’t something he had expected, nor something he had ever physically felt. But suddenly, it mattered. The sperm count was adequate. But only about 1% of the sperm were structurally normal, meaning most were not capable of effective fertilisation. There was increased viscosity, making movement harder. Although motility improved after processing, it could not compensate for poor morphology.
It wasn’t about how many sperm were present. It was about how well they were functioning. And that changed everything.
After IUI Failed
The IUI didn’t work. And the silence after that failure felt heavier than words.
IVF was now the next step. For Swathi, it meant going through intense physical processes again. For Vikram, it meant something harder to express: watching his wife prepare for more, while knowing that his condition would now play an even more critical role.
That awareness brought a different kind of pressure. He had to stay strong for her. But internally there was guilt, responsibility, and a quiet heaviness that kept building. The thought that after everything she had gone through, his report also mattered. He didn’t say it out loud, but he carried it. And unlike her, he didn’t have a space to release it. No place to cry freely, no moment to completely break down. So he held it in, continued to show up, stayed composed, and supported her.
Even when he himself needed support.
💜 Going through something similar? Dr. Suganya works with both partners, not just one. If you’re carrying the weight of a difficult report or a failed cycle, start a conversation on WhatsApp. You don’t have to figure this out alone.
What Brought Them to Fertilia
Somewhere in that phase, they both realised they could not keep going the way they were. Moving from one step to another, addressing things halfway, without understanding the root. They wanted clarity. They wanted to understand what was truly happening in both their bodies.
That decision is what brought them to us.
When they came, we didn’t just see reports. We saw two individuals carrying different forms of the same weight. Her pain visible, his silent. So we approached it differently. Not as her journey alone, but as theirs. We analysed both their reports with equal attention, understanding that his parameters mattered just as much.
Based on that, we prescribed corrections for both. Not as separate plans, but as a shared process.
For Swathi: restoring hormonal balance and correcting deficiencies (low AMH, high prolactin, severely low Vitamin D).
For Vikram: addressing years of a sedentary lifestyle. Long sitting hours, irregular meals, and internal imbalance that was affecting his sperm quality.
The Changes: Nothing Drastic, Just Consistent
Nutritional support became a key part of their journey. Not as a quick fix or something aggressive, but as something consistent. It started with simple changes: a balanced plate, proper portion sizes, meals on time, and conscious nourishment. Nothing complicated, nothing extreme. Just doing the basics right, every single day.
For Vikram, this meant breaking years of unconscious habits. No more skipping meals or long gaps between eating. Instead, simple, nourishing meals eaten on time, every day. Even on busy workdays, even when it felt inconvenient. For Swathi, it meant gently supporting her body, replenishing deficiencies, and helping her system feel safe again.
There was nothing dramatic about these changes. It didn’t feel like a big transformation in the beginning. It was just small, consistent efforts, repeated daily. At times, it felt slow. At times, it felt like nothing was changing. But they continued, because this time it wasn’t about quick results. It was about staying consistent even when progress wasn’t visible.
Vikram didn’t change overnight. There were days he slipped back into old patterns, days when routine felt difficult. But he didn’t stop. He came back to it, again and again, with more awareness each time. Slowly, over weeks, small shifts became noticeable. His energy improved, his body felt more responsive, and the quiet guilt he had been carrying began to ease.
For Swathi, the changes were just as gradual. Her body, which had gone through so much, didn’t respond instantly. But with consistent nourishment and support, a sense of steadiness began to build. There was less overwhelm, less fear, and more calm with each passing cycle.
The Shift
Somewhere along the way, without a clear moment to point to, the journey started to feel different. There was less anxiety, less self-blame, and more understanding. More togetherness. They were no longer just waiting for an outcome. They were actively supporting their bodies every single day.
Vikram felt safe and understood, without any judgment. And that made it easier for him to trust the process and commit to it wholeheartedly.
And it was within this slow, consistent shift that their bodies began to respond.
Over time, with this alignment and patience, their bodies came back into balance in a way that truly supported them. And they conceived naturally.
Not as a sudden moment, but as a result of everything they had been building, day after day.

There was happiness, but more than that, there was relief. A quiet, settled feeling that everything they had been through had finally led them here. No overwhelming reaction, no disbelief. Just a deep sense that their journey had finally begun to move forward.
For Vikram, it wasn’t just about the outcome. It was about knowing that he had shown up, that he had done his part, that he had stood beside her, and also for himself.
In His Own Words
They continued their pregnancy journey with the same care and consistency, staying connected with us throughout. At each stage, they carried forward the same approach they had built. It was no longer just about reaching an outcome, but about maintaining what they had worked towards.
After the delivery, Vikram reached out to share his gratitude:
His words carry the weight of everything they went through: “Because of your support throughout 2025, our pregnancy journey became very beautiful. My wife’s pregnancy went very smoothly because of your care and guidance. You supported us at every stage and even after delivery. You never treated us like patients. You treated us like your own family.”
What This Story Shows
This case study matters because it represents something we don’t talk about enough in fertility care.
Male factor is present in roughly 40-50% of couples facing infertility (Kumar & Singh, 2015, Indian Journal of Urology). Yet in most clinical settings, the focus remains almost entirely on the woman. Her hormones, her cycles, her body. The man gets a semen analysis, and if the count looks fine, the conversation moves on.
But as Vikram’s case demonstrates, count is only one parameter. Morphology, motility, viscosity: these all affect whether conception can happen. And many of these parameters respond to lifestyle changes over a 72-90 day window (the time it takes for new sperm to form).
What made the difference here:
- Both partners were treated equally. Not her journey with him as support, but their journey together.
- Root cause, not just numbers. Vikram’s sedentary lifestyle, irregular eating, and stress were driving his poor morphology. Addressing these changed the outcome.
- Consistency over intensity. No extreme diets or aggressive interventions. Simple changes, done every day, for long enough to matter.
- Emotional safety. Vikram was given space to be a patient too, not just a support system. That trust allowed him to fully commit.
💜 Your fertility journey doesn’t have to be one-sided. Dr. Suganya works with both partners to understand what’s really going on and build a plan that addresses everything, not just one half of the picture. Start a conversation on WhatsApp. It begins with one message.
Frequently Asked Questions
Can teratozoospermia be reversed with lifestyle changes?
In many cases, yes. Sperm take approximately 72 days to form (spermatogenesis cycle), so lifestyle changes need at least 3 months to show results in a repeat semen analysis. Studies show that improvements in diet, reduction of sedentary hours, better sleep, and stress management can meaningfully improve morphology in men with teratozoospermia (Salas-Huetos et al., 2017, Human Reproduction Update). Vikram’s case is one example of this. That said, severe structural causes (genetic, varicocele) may need medical intervention alongside lifestyle changes.
Should both partners be tested and treated in a fertility journey?
Absolutely. Male factor contributes to roughly 40-50% of all infertility cases, yet it’s often underinvestigated. A basic semen analysis is a starting point, but the parameters need careful interpretation. Count alone doesn’t tell the full story. Morphology, motility, viscosity, and even the man’s metabolic health all play a role. At Fertilia, we assess and prescribe for both partners from the very first consultation.
What does 1% normal morphology actually mean?
It means that out of 100 sperm examined under strict criteria (Kruger’s), only 1 had a structurally normal head, midpiece, and tail. The WHO reference value is 4% or higher. Low morphology (teratozoospermia) doesn’t mean conception is impossible, but it significantly reduces the chances because abnormally shaped sperm have difficulty penetrating and fertilising an egg. The good news is that morphology can improve with targeted lifestyle changes over 3 months.
Why did IUI fail if the sperm count was normal?
IUI works best when both motility and morphology are adequate. In Vikram’s case, while count was normal (50 million total in the IUI sample), only 1% had normal morphology, and progressive motility was slightly below reference. Even after washing and concentrating the sample, the proportion of functionally capable sperm was too low. This is why a semen analysis needs to be interpreted as a whole picture, not just one number.
How does a sedentary lifestyle affect sperm quality?
Prolonged sitting increases scrotal temperature, which is one of the most well-documented factors affecting sperm production and morphology. Additionally, a sedentary lifestyle is associated with higher BMI, insulin resistance, oxidative stress, and lower testosterone, all of which impact semen parameters. For Vikram, years of desk-bound work with irregular meals created a compounding effect that showed up clearly in his report. Regular movement, even walking, and consistent nutrition were key parts of his recovery.
Can diet alone improve sperm morphology?
Diet is one important factor but usually not sufficient on its own. The research supports a combined approach: anti-inflammatory nutrition (fruits, vegetables, whole grains, nuts, fish), regular physical activity, adequate sleep (7-8 hours), reduced alcohol, no smoking, and stress management. Specific nutrients like zinc, selenium, folate, vitamin C, vitamin E, and omega-3 fatty acids have evidence supporting their role in semen quality (Salas-Huetos et al., 2017). At Fertilia, the nutrition plan is always part of a broader lifestyle prescription.
How long does it take to see improvement in semen analysis results?
The spermatogenesis cycle is approximately 72 days, so any lifestyle intervention needs a minimum of 3 months to reflect in a repeat semen analysis. Some men see improvements earlier, but a meaningful, reliable comparison requires that full cycle. This is why our program runs for 90 days: it’s designed around this biological timeline. Patience and consistency during this window are what made the difference for Vikram and Swathi.
This is the sixth in our series of patient case studies from our clinic. Every story is real, verified, and shared with the patient’s explicit consent. Names and identifying details are changed to protect privacy.
Related Reading
- Semen Analysis: What Your Report Really Means
- IUI vs IVF: When Do You Really Need It?
- How to Prepare Your Body for IUI or IVF
- How Deepa Conceived Naturally with AMH 0.62
- How to Get Pregnant Fast: Evidence-Based Guide, timing, nutrition and lifestyle steps for natural conception
- 7 Evidence-Based Ways to Boost Fertility Naturally
💜 Every couple’s journey is different. Yours deserves personal attention. Talk to Dr. Suganya on WhatsApp and take the first step together.





