Names have been changed to protect patient privacy. Clinical details are shared with the patient’s consent.
When Madhu reached out to us, she was carrying more than just extra weight. She was carrying the grief of a failed embryo transfer, the anxiety of another one approaching in just a month, and a quiet, persistent question: “Will my body be able to support this pregnancy?”
She was 36. Tired, but still holding on.
She had already been through multiple IUI attempts and one embryo transfer that did not succeed. Now she was standing at a very sensitive point in her journey. The next transfer was weeks away.
This time, she did not want to leave anything to chance.
The Situation
Madhu came to us not because she had given up on IVF. She came because she wanted to give her body the best possible chance of supporting the embryo transfer. She wanted to walk into that procedure prepared.
Madhu’s profile:
- Age: 36
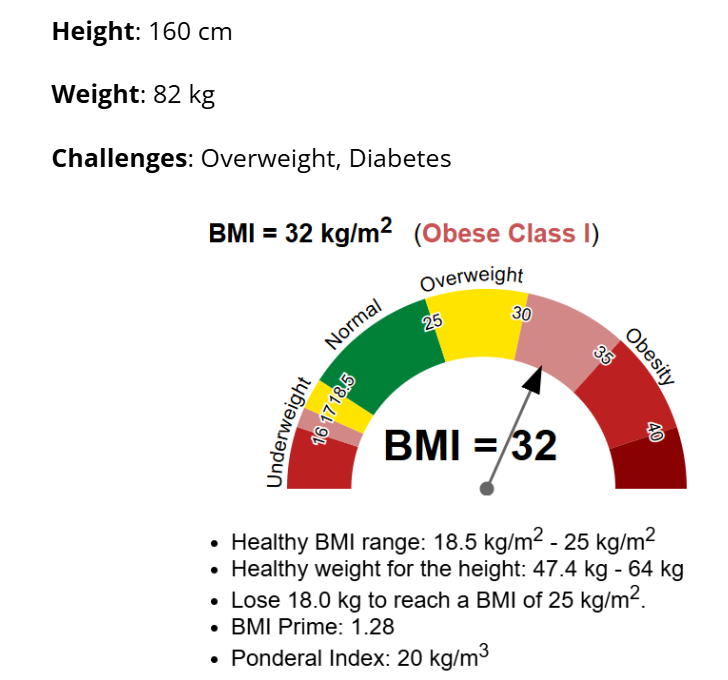
- Height: 160 cm
- Weight: 82 kg (BMI: 32, Obese Class I)
- HbA1c: 6.3% (pre-diabetic range, above the 5.7% non-diabetic threshold)
- Fasting glucose: 107 mg/dL (pre-diabetic: 100-125)
- Post-meal glucose: 160.6 mg/dL (pre-diabetic: 140-199)
- Total cholesterol: 209 mg/dL (borderline high)
- LDL cholesterol: 146.4 mg/dL (borderline high)
- HDL cholesterol: 46.1 mg/dL (low, desirable is 60+)
- Previous attempts: Multiple IUI cycles, one failed embryo transfer
Her initial BMI assessment made it clear: her metabolic health needed urgent attention before the transfer.
Her HbA1c of 6.3% confirmed she was in the pre-diabetic zone:

And her cholesterol profile showed borderline high total cholesterol at 209 mg/dL with elevated LDL:
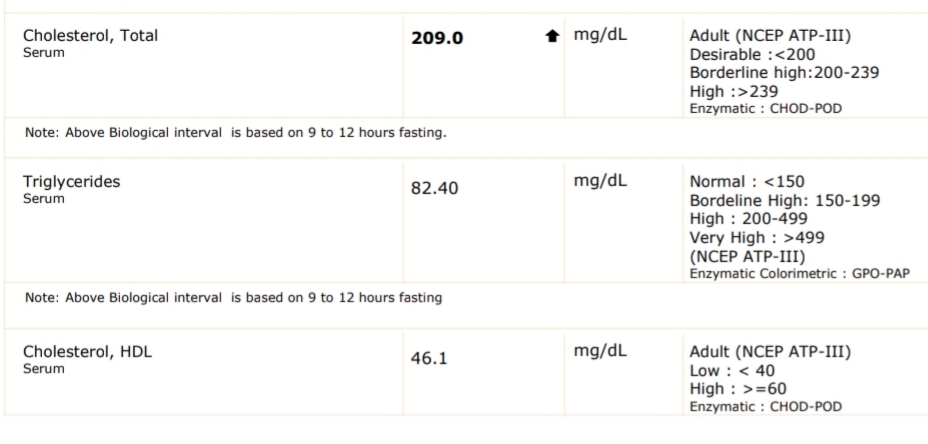

More than the numbers, it was the reality behind them. Elevated blood sugar and insulin resistance can directly affect embryo implantation. Research shows that women with pre-diabetic glucose levels have lower IVF success rates, partly because hyperglycaemia impairs endometrial receptivity (Orvieto et al., 2014, Reproductive BioMedicine Online). Her fasting glucose of 107 and post-meal glucose of 160.6 were both in ranges that warranted immediate action.


She came to us with one clear intention: “Help me prepare my body the right way.”
Are You Preparing for IVF or an Embryo Transfer?
If you want to give your body the best possible chance before a procedure, we can help you understand what lifestyle changes actually matter.
Why Metabolic Health Matters Before IVF
Many women going through IVF are told to rest and eat well, but not told how. General advice like “eat healthy” or “reduce stress” is well-intentioned, but without specifics and daily guidance, it stays vague.
Here is what research tells us about why metabolic preparation matters:
1. Blood sugar affects implantation Elevated glucose levels create a hostile environment for embryo implantation. The endometrial lining is sensitive to metabolic signals, and chronically elevated insulin can alter the immune and hormonal environment needed for successful implantation (Gu et al., 2021, Frontiers in Endocrinology).
2. Weight affects IVF outcomes A BMI above 30 is associated with lower live birth rates in IVF cycles. This is not about appearance. It is about the metabolic, hormonal, and inflammatory environment that the embryo is entering (Rittenberg et al., 2011, Human Reproduction Update).
3. Cholesterol matters more than most people realise Cholesterol is the building block for steroid hormones, including progesterone, which is critical for maintaining early pregnancy. Abnormal lipid profiles can disrupt the hormonal balance needed to sustain implantation (Schisterman et al., 2014, Human Reproduction).
Madhu’s profile checked every one of these boxes. Her metabolic environment needed attention before the next transfer.
The Plan
We had roughly one month before her embryo transfer. There was no time for vague plans or complicated protocols. Everything had to be specific, practical, and sustainable.
We designed a programme around three daily pillars: food, movement, and monitoring.
Daily sugar monitoring
This was the foundation. Madhu checked her fasting and post-meal blood sugar at home every single day using a glucometer. She shared the readings with our team daily.
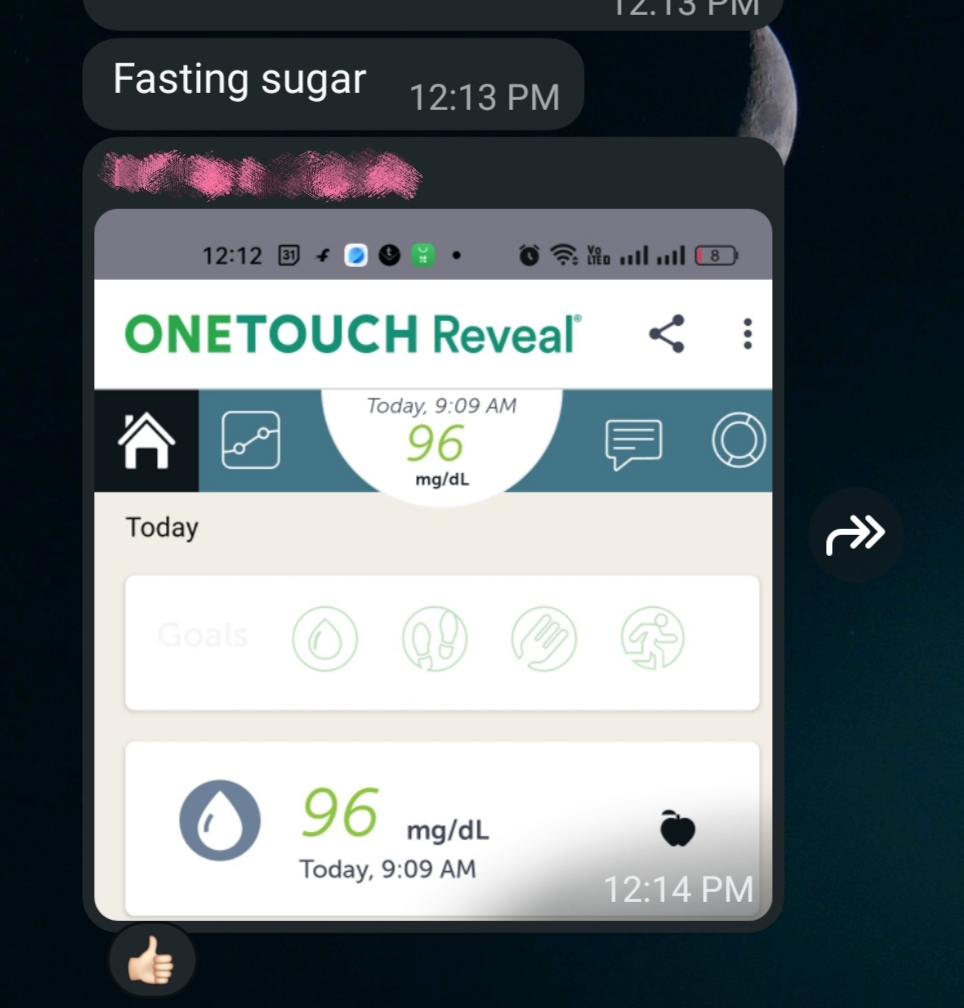
We did not wait for monthly lab reports. We watched her body respond in real time and adjusted her plan instantly when needed. If a reading spiked after a particular meal, we knew by the next morning and could course-correct the same day.
Balanced, nourishing Indian meals
We did not put Madhu on a restrictive diet. Restriction signals scarcity to the body, and a body preparing for pregnancy needs to feel nourished, not deprived.
Instead, we gave her meal plates that were:
- Built around Indian foods she already cooked: ragi, millet upma, dal, green moong, dahi, vegetables
- Balanced for blood sugar stability (complex carbs + protein + fibre at every meal)
- Timed properly (consistent meal timing helps regulate glucose response)
- Simple enough to follow daily without extra effort



Every meal was designed to keep her blood sugar stable while giving her body the nourishment it needed for what lay ahead.
Consistent walking
No gym. No intense workouts. Just consistent, daily movement.
Madhu built her walking habit gradually and reached 10,000 to 12,000 steps per day. Some days, she hit over 14,000.

Not sometimes. Not occasionally. Every single day.
Walking is one of the most effective ways to improve insulin sensitivity. A 2019 meta-analysis in Diabetes Care found that even moderate-intensity walking significantly reduces fasting glucose and HbA1c in pre-diabetic individuals (Qiu et al., 2019). For Madhu, it was the perfect fit: low-impact, sustainable, and something she could do even during the two-week wait after her transfer.
Daily check-ins
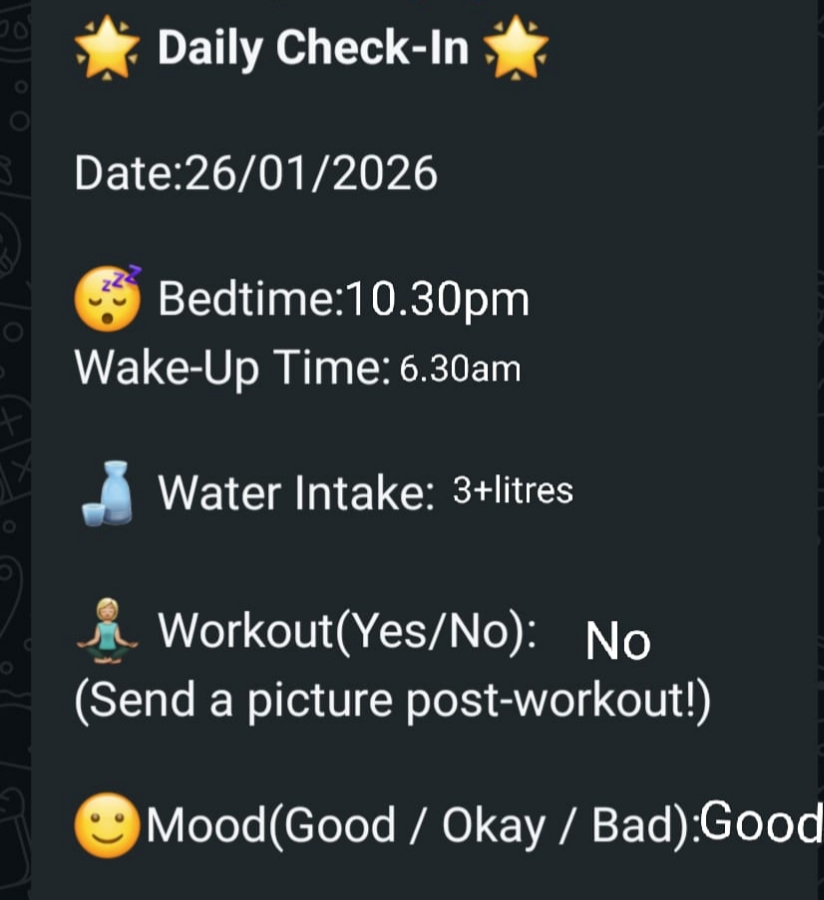
Every day, Madhu filled out a structured check-in with our team, covering her sleep, water intake, mood, and whether she had walked.
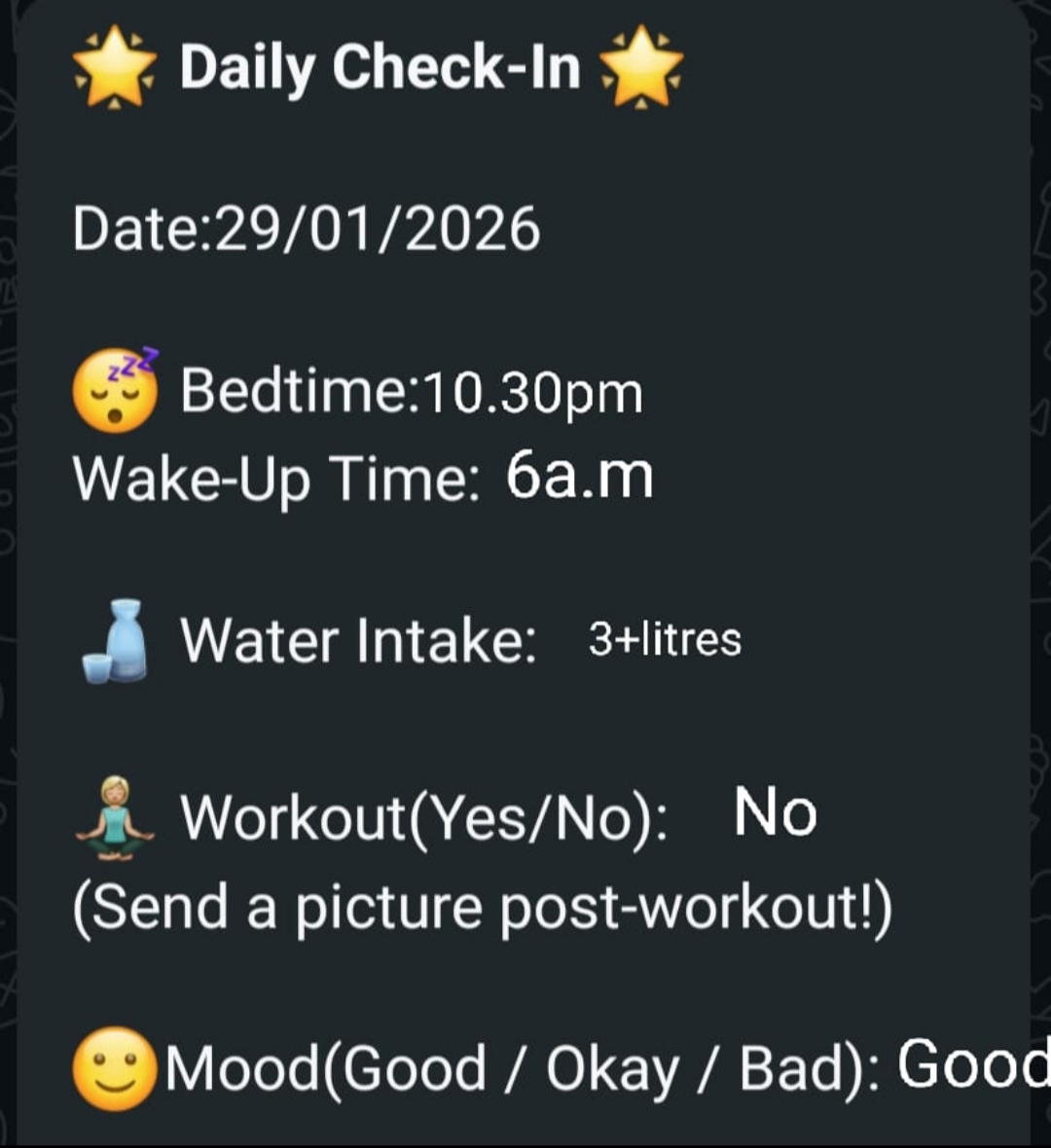
This was not just data collection. It was a daily touchpoint, a way for Madhu to feel that someone was walking this journey alongside her. Every reading was reviewed. Every question was answered. She was never left to figure things out on her own.
The Journey
Week by week, her body responded
Within the first few weeks, the changes started showing in her numbers.
Her fasting glucose, which had been 107 mg/dL (pre-diabetic), dropped to 96 mg/dL (normal).
Her post-meal glucose, which had been 160.6 mg/dL, dropped to 96 mg/dL. That is a remarkable improvement, moving from the pre-diabetic range into a completely healthy range.

Her weight dropped from 82 kg to 76.7 kg, a loss of approximately 6 kg.

What changed inside
But the transformation was not just in the numbers. Madhu described feeling lighter, calmer, and more in control. The daily routine of walking, eating well, monitoring her sugars, and checking in with the team gave her something she had not felt during her previous transfer attempt: a sense of agency.
She was not just waiting for the procedure to work. She was actively preparing her body. And that shift in mindset made a real difference.
The embryo transfer
When the day came for her second embryo transfer, Madhu walked into the clinic prepared. Her blood sugar was under control. Her weight had come down meaningfully. Her metabolic profile was in a far better place than it had been weeks ago.
This time, the transfer succeeded.
She conceived.
We stayed
But for us, that was not the end.
We did not step back after the positive result. We continued supporting Madhu through her early pregnancy, guiding her on diet during pregnancy, helping her understand the changes that happen after IVF, supporting her with safe walking and daily routines, and staying connected to answer every question.
Because pregnancy after IVF, especially after a previous failed transfer, needs even more care, more reassurance, and more consistent guidance.
Today, Madhu is 12 weeks pregnant and doing well.
The Results
| Metric | Before | After |
|---|---|---|
| Weight | 82 kg (BMI 32) | 76.7 kg (approximately 6 kg lost) |
| Fasting glucose | 107 mg/dL (pre-diabetic) | 96 mg/dL (normal) |
| Post-meal glucose | 160.6 mg/dL (pre-diabetic) | 96.0 mg/dL (normal) |
| HbA1c | 6.3% (pre-diabetic) | Significantly improved |
| Daily steps | Minimal | 10,000-14,000 |
| Embryo transfer | Previously failed | Successful |
| Pregnancy | Multiple failed attempts | Currently 12 weeks |
In Her Own Words
“I want to express my heartfelt gratitude for the wonderful experience I’ve had with Fertilia under your guidance. Over the past three months, I’ve lost 6 kgs and seen a significant improvement in my HbA1c. The thoughtful consultations and caring follow-ups truly helped me in reducing my blood sugar.
What makes me especially happy is that this progress came naturally, simply by balancing my food choices and walking regularly, without any medicines. Fertilia has inspired me to maintain a healthy lifestyle, and I feel motivated to continue this journey.
A special thanks to Dr. Suganya mam and Ilakiya mam for their guidance and genuine care.”
What This Case Study Teaches Us
1. IVF is not just about the procedure. It is about the body receiving it.
The embryo transfer is one moment. But the metabolic environment that the embryo enters has been building for weeks and months. Optimising blood sugar, weight, and cholesterol before a transfer gives the embryo the best possible conditions for implantation.
2. “Rest and eat well” is not enough guidance
Women going through IVF are often told to rest, eat well, and avoid stress. But without a specific preparation plan, daily monitoring, and someone to guide them through it, this advice stays abstract. Madhu’s success came from specifics: exact meal plates, daily sugar readings, step counts, and a team reviewing everything in real time.
3. Daily monitoring changes everything
When you check your blood sugar every day and share it with your care team, two things happen. First, you see your body respond to the changes you are making. That is motivating. Second, your team can make instant adjustments instead of waiting for a monthly lab report. This real-time feedback loop is what made Madhu’s one-month timeline possible.
4. Lifestyle support and IVF work together
This is not a story about choosing between lifestyle changes and IVF. It is a story about combining them. Madhu’s fertility specialist handled the medical procedure. We handled the metabolic preparation. Together, the outcome was better than either approach alone. Research supports this: a 2020 systematic review in Human Reproduction Update found that lifestyle interventions before IVF improve clinical pregnancy rates (Lim et al., 2020).
5. The daily connection matters as much as the plan
Madhu’s testimonial does not mention a specific diet tip or exercise routine. She talks about “thoughtful consultations,” “caring follow-ups,” and “genuine care.” When you are going through something this emotionally intense, knowing that someone is truly walking with you, every single day, changes the experience entirely.
Preparing for IVF? Let Us Help.
Every woman’s situation is different. Whether you are going through your first IVF cycle or preparing for another embryo transfer, optimising your metabolic health beforehand can make a meaningful difference. We work alongside your fertility specialist to ensure your body is in the best possible condition.
Frequently Asked Questions
Does weight loss before IVF improve success rates?
Yes. Research consistently shows that even a 5-10% reduction in body weight can improve IVF outcomes in women with elevated BMI. A meta-analysis by Rittenberg et al. (2011, Human Reproduction Update) found that obesity is associated with lower live birth rates in IVF. Madhu’s 6 kg loss (approximately 7% of her body weight) brought her into a more favourable metabolic range before her transfer.
How does blood sugar affect embryo implantation?
Elevated blood sugar and insulin resistance can impair endometrial receptivity, which is the lining’s ability to accept and support an embryo. High glucose levels also increase oxidative stress and inflammation in the uterine environment. Bringing fasting and post-meal glucose into normal ranges, as Madhu did, creates a more hospitable environment for the embryo. Women who develop elevated blood sugar during pregnancy may also face gestational diabetes, making pre-conception glucose control even more important.
Can lifestyle changes really make a difference in just one month?
Certain metabolic markers respond quickly to consistent changes. Fasting glucose and post-meal glucose can improve within weeks with the right dietary changes and regular walking. Weight loss of 1-2 kg per week is achievable and sustainable with balanced nutrition (not extreme restriction). The key is consistency, which is why daily monitoring and daily check-ins with a care team matter so much.
Should I follow a special diet before IVF?
Rather than a “special” diet, the goal is a balanced, nourishing eating pattern that keeps your blood sugar stable and provides the nutrients your body needs. This means regular meals with complex carbohydrates (ragi, millets, whole grains), adequate protein (dal, paneer, eggs, dahi), plenty of vegetables, and healthy fats. Avoid extreme restriction. Your body needs to feel nourished, not stressed, before a transfer.
Can I exercise during IVF preparation?
Moderate exercise, especially walking, is both safe and beneficial during IVF preparation. Walking improves insulin sensitivity, reduces stress, and supports healthy weight management. Madhu walked 10,000-14,000 steps daily throughout her preparation. After the embryo transfer, exercise recommendations may change (your fertility specialist will advise). But in the weeks leading up to a transfer, consistent movement is one of the best things you can do.
Does Fertilia replace my IVF doctor?
Not at all. We work alongside your fertility specialist, not in place of them. Your doctor handles the medical procedure (stimulation, retrieval, transfer). We handle the lifestyle preparation: nutrition, movement, blood sugar management, and daily support. The two approaches complement each other. Madhu’s fertility specialist handled her embryo transfer while we ensured her body was metabolically prepared for it.
How is Fertilia’s IVF support different from general advice?
Three things set it apart. First, it is doctor-supervised: Dr. Suganya is an OB-GYN with 15+ years of experience who reviews your health profile and personalises the plan. Second, it is daily: you are not given a plan and left alone. You have daily check-ins, real-time sugar monitoring, and a team that responds to every reading. Third, it continues after the transfer: we do not stop when the procedure happens. We support you through early pregnancy and beyond.
Related Case Studies
- How Gowri went from HbA1c 9.8 to pregnancy. Another “doctor referred her to us first” story. Gowri was sent to Fertilia with PCOS, HbA1c 9.8%, and a BMI of 38. She conceived in one cycle of ovulation induction after 3 months of metabolic preparation.
- How a couple prepared for IVF together and formed 3 embryos. A couple’s joint preparation: PCOS plus cardiac history, 35 kg lost, 3 embryos formed.
This is part of a series of patient case studies from our clinic. Every story is real, verified, and shared with the patient’s explicit consent. Names and identifying details are changed to protect privacy.
Dr. Suganya Venkat is an OB-GYN with 15+ years of experience. She holds an MBBS (SRMC, 5 Gold Medals), MD in Pathology (CMC Vellore), and DNB in OB-GYN (GKNM Hospital, Coimbatore).





