Names have been changed to protect patient privacy. Clinical details are shared with the patient’s consent.
When Shalini came to us, she was not in panic. She was not breaking down. She was carrying something quieter and heavier — a silent hope that maybe this time, someone would look deeper.
She was 29. Married for three years. Both she and her husband worked in IT. By every conventional measure, she was young and healthy. And yet, for three years, not a single positive pregnancy test.
Two IUI cycles had already failed. Her doctors had told her clearly: the next step was IVF, and she should consider it before her egg reserve came down further.
But Shalini was not ready for that step yet. She wanted to try one more thing. She wanted to understand what was actually happening in her body, and whether there was something that could still be done differently.
That is when she found Fertilia.
The Situation
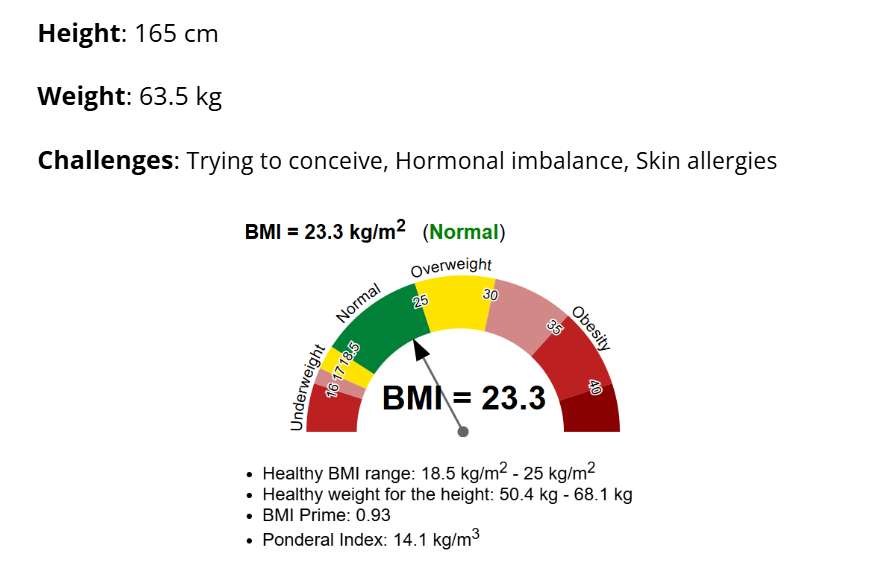
On paper, Shalini’s case looked straightforward. Regular menstrual cycles. No major hormonal complaints. A BMI of 23.3 — perfectly normal.
Shalini’s profile:
- Age: 29
- Height: 165 cm
- Weight: 63.5 kg (BMI: 23.3, normal)
- AMH: 1.77 ng/mL (low-satisfactory range)
- Cycles: Regular
- Previous attempts: 2 failed IUI cycles (November and January)
- Other conditions: Psoriasis (on treatment since 2025), with persistent skin allergies
Her blood reports came back normal. Her husband’s reports were normal too.
If you stopped here, you might think nothing was wrong.
But we did not stop here.
What the Scan Revealed
When we looked at her ultrasound, the picture changed entirely.

The scan showed:
- Right ovary: Massively enlarged — 6.7 x 4.4 x 4.5 cm, volume 70 mL (a normal ovary is around 6-10 mL)
- Endometriotic cyst: 4.0 x 3.4 x 4.1 cm, volume 30 mL
- Another simple cyst in the right ovary: 3.2 x 1.7 cm
- Left ovary: Normal in size (3.2 x 1.8 x 1.9 cm, volume 6 mL)
- Both ovaries were stuck to the back of the uterus
That last line is critical. When both ovaries are stuck to the uterus through adhesions, it creates a significant anatomical barrier to natural conception. The fallopian tubes may not be able to pick up the released egg properly. The egg’s journey from ovary to tube to uterus — the most basic requirement for natural conception — is physically disrupted.
This is what makes endometriosis and fertility such a complex picture. The condition does not just cause pain. It silently changes the anatomy of the reproductive organs, making conception difficult even when everything else looks normal on a blood report.

Her AMH of 1.77 ng/mL sat in the lower end of the satisfactory range. Not critically low, but not optimal either. Combined with the endometriotic cyst and the anatomical distortion, the clinical picture was clear: natural conception was going to be very difficult. Her doctors were not wrong when they recommended IVF.
But Shalini wanted to try something different first. And we believed there was room to try.
Have You Been Told IVF Is Your Only Option?
If you have endometriosis and have been advised to move directly to IVF, it may be worth exploring whether lifestyle-based support can help your body first. Every woman’s situation is different, and we can help you understand your full picture.
Why an Anti-Inflammatory Diet Matters for Endometriosis
Before we explain the plan, it helps to understand why nutrition is central to managing endometriosis.
Endometriosis is fundamentally an inflammatory condition. The endometrial-like tissue growing outside the uterus triggers a chronic inflammatory response. This inflammation does not stay local — it affects the entire pelvic environment, including the ovaries, fallopian tubes, and the peritoneal fluid that surrounds them.
Research increasingly shows that dietary patterns can influence this inflammatory environment:
1. Anti-inflammatory diets reduce key inflammatory markers in endometriosis
A 2022 evidence review published in Nutrients found that anti-inflammatory dietary patterns — rich in omega-3 fatty acids, fruits, vegetables, and whole grains — are associated with reduced inflammation and improved fertility outcomes in women with conditions like endometriosis (Alesi et al., 2022, Nutrients).
2. Dietary interventions show promise for endometriosis symptom management
A systematic review in Reproductive Sciences examined the effectiveness of dietary interventions in treating endometriosis. While the authors noted that more high-quality studies are needed, the existing evidence supports the role of dietary modification as a complementary approach, particularly in reducing oxidative stress and inflammation — two drivers of endometriosis progression (Nodler et al., 2020, Reproductive Sciences).
3. Specific foods influence the endometriosis inflammatory cycle
A 2025 review in Frontiers in Nutrition explored how dietary patterns and nutritional supplementation affect endometriosis management. The evidence points to diets rich in antioxidants, fibre, and anti-inflammatory compounds helping to modulate the oxidative stress and chronic inflammation that characterise the condition (Frontiers in Nutrition, 2025).
This is why we did not just tell Shalini to “eat healthy.” We designed a specific endometriosis-friendly anti-inflammatory diet plan.
The Plan
Our approach for Shalini had three pillars: an endometriosis-specific anti-inflammatory diet, consistent yoga practice, and careful ovulation tracking.
Anti-inflammatory, endometriosis-friendly meals
We did not put Shalini on a restrictive diet. Her weight was already normal. The goal was not weight loss — it was reducing the inflammatory environment in her pelvis and supporting her body’s ability to heal.
Every meal was built around:
- Anti-inflammatory Indian foods: Haldi (turmeric), which contains curcumin — a well-studied anti-inflammatory compound. Fresh vegetables. Legumes. Whole grains.
- High-fibre, plant-rich plates to help regulate oestrogen metabolism. Excess oestrogen fuels endometriosis, and fibre helps the body clear it efficiently.
- Protein at every meal from dal, legumes, eggs, and peanuts to support tissue repair and immune function.
- Avoiding pro-inflammatory triggers: Processed foods, excess refined sugar, and deep-fried items that can worsen the inflammatory cycle.



These were not elaborate meals. They were simple, home-cooked Indian plates that Shalini could prepare even during a hectic week. The consistency mattered more than the complexity.
Daily yoga
Even though Shalini’s weight was normal, we prioritised daily movement. With endometriosis, movement is not about burning calories — it is about reducing inflammation, improving blood flow to the pelvic region, and managing the stress that comes with years of trying.
Shalini chose yoga. And she never missed it.

She combined her yoga with early morning sunlight exposure for vitamin D — a nutrient that plays a role in immune regulation and inflammation management. Research has linked vitamin D deficiency with endometriosis severity (Anastasi et al., 2017, Reproductive Biology and Endocrinology).
Ovulation tracking and fertile window guidance
We tracked Shalini’s cycle carefully, helping her and her husband understand her fertile window and optimise timing. After three years of trying without guidance on cycle timing, this structured approach gave them clarity on something that had been left to chance.
The Journey
Shalini followed the plan with remarkable consistency. There was no resistance. No overthinking. Just trust and daily effort.
The first change: her skin
Within the first month, something unexpected started improving. Her skin allergies — the chronic, persistent condition she had been dealing with alongside her psoriasis — began to calm down.
Not completely gone overnight. But slowly reducing. Becoming manageable.
For Shalini, that itself felt like a relief. Her body was responding. The anti-inflammatory approach was working on more than just her reproductive system — it was helping her whole body.
Life got hectic
Around the same time, Shalini and her husband were going through a major life change. They were shifting houses, moving from one state to another. New place. New routine. The kind of physical and emotional upheaval that can throw everything off.
Through all of this, we stayed connected. We continued tracking her cycle. We continued guiding her meals. We continued answering every question.
The delayed period
Then, something stood out. Her period got delayed. Ten days.
When we spoke to her, she casually mentioned something: “I’ve been feeling very hungry… and a little more tired than usual.”
That small detail made us pause.
We gently asked her to take a pregnancy test. But she hesitated. After trying for three years, after seeing negative results again and again, it is not easy to believe that this time could be different.
Still, we encouraged her. Just once. Just to be sure.
She took the test.
Two lines
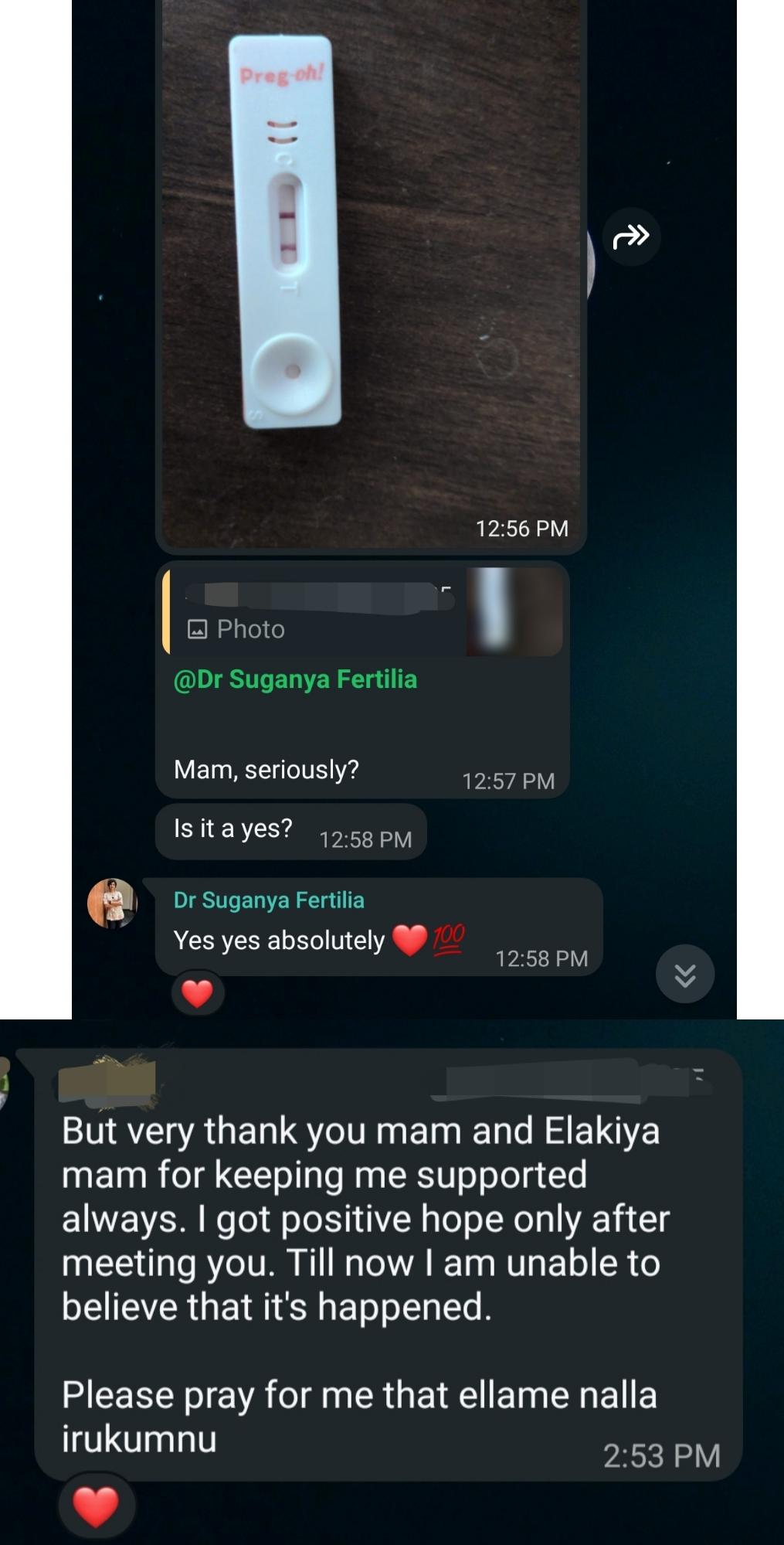
For a moment, she could not believe it. Even saying it out loud felt unreal.
After three years of trying. After two failed IUI cycles. After being told IVF was her only option.
She had conceived. Naturally. In approximately 45 days on the program.
The cyst surprise
The very next day, we asked her to visit her doctor for a confirmation scan. And when the scan results came, they brought another unexpected finding.
The endometriotic cyst — which had been 4 cm earlier — had reduced to around 2 cm.
In just about one and a half months, her body had not only supported a pregnancy. It had also started healing itself. The anti-inflammatory approach was not just managing symptoms — it was creating an environment where her body could repair.
The Results
| What | Before | After (~45 days) |
|---|---|---|
| Trying to conceive | 3 years, 0 pregnancies | Conceived naturally |
| IUI attempts | 2 failed cycles | Not needed |
| IVF | Recommended as next step | Not needed |
| Endometriotic cyst | 4.0 x 3.4 x 4.1 cm (30 mL) | Reduced to ~2 cm |
| Skin allergies | Chronic, persistent | Significantly improved |
| Ovaries | Both stuck to back of uterus | Pregnancy achieved despite adhesions |
| Outcome | IVF was the only option left | Natural conception |
In Her Own Words
“But very thank you mam and Elakiya mam for keeping me supported always. I got positive hope only after meeting you. Till now I am unable to believe that it’s happened. Please pray for me that ellame nalla irukumnu.”
What This Case Study Teaches Us
1. Endometriosis with anatomical difficulty does not automatically mean IVF is the only path
Shalini had every reason to go directly to IVF. A 4 cm endometriotic cyst. Both ovaries stuck to the uterus. Two failed IUI cycles. An AMH on the lower side. Her doctors were not wrong to recommend IVF — it was a valid clinical option.
But before taking that step, there was room to address something that had not been addressed: the inflammatory environment driving her endometriosis. When we supported her body with the right nutrition, movement, and daily guidance, it responded in ways that surprised everyone — including us.
This is not to say that IVF is unnecessary for endometriosis. For many women, it is the right choice. But for women who want to explore what lifestyle-based support can do first, Shalini’s story shows that it is worth trying.
2. Anti-inflammatory nutrition is not optional for endometriosis — it is foundational
Endometriosis is an inflammatory condition. Every meal either adds to that inflammation or helps reduce it. Shalini’s diet was not a supplement to her treatment. It was central to it. The fact that her cyst reduced by approximately 50% in 45 days, alongside the dietary changes, underlines how much the body can respond when inflammation is actively managed through food.
3. Normal weight does not mean normal inflammation
Shalini’s BMI was 23.3 — perfectly healthy. Many women (and sometimes doctors) assume that if weight is normal, there is nothing to fix through diet. But weight and inflammation are not the same thing. You can have a healthy BMI and still have a body running on chronic inflammation, especially with an autoimmune condition like psoriasis alongside endometriosis. The improvement in her skin allergies confirmed this: the anti-inflammatory diet was addressing systemic inflammation, not just weight.
4. Normal blood reports do not tell the whole story
Shalini’s blood work was normal. Her husband’s reports were normal. If the investigation had stopped at blood tests, the endometriotic cyst, the ovarian adhesions, and the anatomical barriers to conception would have remained invisible. This is why a thorough assessment — including detailed ultrasound — matters, especially when conception is not happening despite everything looking “fine” on paper.
5. Consistency matters more than perfection
Shalini was moving houses. Shifting states. Dealing with the stress of relocation. She did not have perfect conditions. But she had consistency. She followed her meal plan. She did her yoga every morning. She stayed in touch with our team every day. In fertility, consistency over weeks matters far more than perfection on any single day.
Thinking About IVF? Consider This First.
If you have endometriosis and are weighing your options between continuing naturally and moving to IVF, Fertilia’s program may help you prepare your body either way. Whether you conceive naturally (as Shalini did) or proceed to IVF with a healthier, less inflamed body, the preparation is never wasted.
Frequently Asked Questions
Can you conceive naturally with endometriosis?
Yes. While endometriosis makes conception more challenging, many women with endometriosis conceive naturally, especially with the right support. The key factors are the severity of the disease, the extent of adhesions, and the overall inflammatory environment. Shalini conceived naturally despite a 4 cm endometriotic cyst and both ovaries stuck to her uterus — a situation where natural conception was considered very unlikely.
What should I eat if I have endometriosis and am trying to conceive?
An anti-inflammatory diet is foundational. Focus on foods rich in omega-3 fatty acids, antioxidants, and fibre. Indian foods like haldi (turmeric), fresh vegetables, dal, whole grains, beetroot, and green leafy vegetables are excellent choices. Avoid processed foods, excess refined sugar, and deep-fried items that can worsen inflammation. A 2022 review in Nutrients found that anti-inflammatory dietary patterns are associated with improved fertility outcomes (Alesi et al., 2022).
What happens after 2 failed IUI cycles with endometriosis?
After two failed IUI cycles, most fertility specialists recommend considering IVF, especially if there is a structural issue like an endometriotic cyst or adhesions. This is a valid recommendation. However, some women choose to explore lifestyle-based support before IVF to address inflammation and optimise their body’s environment. Shalini chose this path and conceived naturally. The right choice depends on your specific situation, your age, your AMH levels, and your personal preferences.
Can an endometriotic cyst reduce without surgery?
Endometriotic cysts (endometriomas) are typically managed through medication or surgery. However, anti-inflammatory dietary and lifestyle interventions may contribute to reducing the inflammatory environment that supports cyst growth. In Shalini’s case, her cyst reduced from 4 cm to approximately 2 cm over about 45 days while she was on an anti-inflammatory diet and yoga program. While this is a single case and not a guarantee, it aligns with research showing that dietary interventions can modulate the inflammatory processes involved in endometriosis (Nodler et al., 2020, Reproductive Sciences).
Is it worth trying a lifestyle program before IVF?
For many women, yes. A lifestyle program before IVF is not an either/or decision. If you conceive naturally (as Shalini did), that is the best outcome. If you do not conceive naturally but have reduced inflammation, improved your nutrition, and optimised your body’s environment, you are going into IVF in a significantly better position. Research shows that lifestyle interventions before IVF improve clinical pregnancy rates (Lim et al., 2020, Human Reproduction Update). Either way, the preparation is never wasted.
Does yoga help with endometriosis and fertility?
Yoga can be beneficial for endometriosis management. It helps reduce stress (elevated cortisol can worsen inflammation), improves blood flow to the pelvic region, and supports overall well-being. Shalini practised yoga daily throughout her program and combined it with morning sunlight exposure for vitamin D. While yoga alone is unlikely to resolve endometriosis, as part of a comprehensive anti-inflammatory program, it contributes meaningfully to creating a healthier environment for conception.
How long does Fertilia’s program take to show results for endometriosis?
Every woman’s body responds differently. Shalini conceived within approximately 45 days, which was faster than expected given her clinical picture. Some women see improvements in symptoms within the first month, while conception may take longer depending on the severity of endometriosis and other factors. The program is typically structured as a 90-day program, with ongoing assessment and adjustments throughout.
This is part of a series of patient case studies from our clinic. Every story is real, verified, and shared with the patient’s explicit consent. Names and identifying details are changed to protect privacy.
Dr. Suganya Venkat is an OB-GYN with 15+ years of experience. She holds an MBBS (SRMC, 5 Gold Medals), MD in Pathology (CMC Vellore), and DNB in OB-GYN (GKNM Hospital, Coimbatore).





